The aim of this study was to describe oral lesions in a group of patients with COVID-19. We recruited 55 patients, 25 women (45.5%) and 30 men (54.5%), aged between 1 and 89 years with confirmed COVID-19 at different stages of severity. After obtaining informed consent, we examined their mouths and recorded clinical findings. Forty percent of the patients had at least 1 oral lesion. The most common lesions were candidiasis and ulcers (7 patients each); 2 patients had enanthems. Geographic tongue and caviar tongue were also observed. Altered taste, dry mouth, and painful/burning mouth were noted in 60%, 27.3%, and 36.4% of patients, respectively. Oral mucosal alterations and lesions were prevalent in this series of COVID-19 patients. Altered taste and a painful/burning mouth were common symptoms.
El propósito de este trabajo fue caracterizar las alteraciones orales en un grupo de pacientes COVID-19. Para ello se evaluaron 55 pacientes hospitalizados, confirmados COVID-19 en distintos estadios de severidad. Previo consentimiento informado, se examinó la cavidad oral y se registraron los hallazgos clínicos. El grupo de estudio estuvo conformado por 25 mujeres (45,5%) y 30 hombres (54,5%), con edades comprendidas entre 1 y 89 años. Un 40% de los pacientes mostraron alguna lesión bucal. Las lesiones más comunes fueron candidiasis y ulceraciones (7 pacientes cada uno) y en dos pacientes se observó enantema. También se encontraron alteraciones de la normalidad como glositis migratoria y varicosidades linguales. Asimismo, se registraron alteraciones del gusto, xerostomía y dolor/ardor bucal en el 60%, 27,3% y 36,4% respectivamente. En los pacientes COVID-19 se observaron con frecuencia alteraciones y lesiones en la mucosa bucal. Finalmente, la disgeusia y el dolor y/o el ardor oral fueron síntomas comunes en estos pacientes.
Over the course of the pandemic, a range of COVID-19 presentations affecting various systems, including the skin and mucous membranes, have been described. Lesions of the oral mucosa have been described in few studies,1 and it remains unclear whether they are a consequence of COVID-19 treatments, immune alterations caused by the virus, or other factors such as the high levels of stress associated with infection. The presence in the oral mucosa of angiotensin-converting enzyme 2 (ACE2) and transmembrane protease serine 2 (TMPRSS2) receptors,2,3 and of the viral spike protein,4 suggests a direct effect of the virus in some of the observed oral manifestations.
The oral manifestations described in COVID-19 patients are varied, although many have been previously described as secondary clinical signs in other diseases. A recent study of 666 patients carried out in Spain reported oral lesions in more than 25% of patients. These included inflammation of the lingual papillae, glossitis with lateral indentations, aphthous stomatitis, mucositis, and glossitis with patchy depapillation (migratory glossitis).5
Other lesions such as enanthem,6 ulcerations,7,8 vascular and hemorrhagic lesions,9,10 candidiasis,11,12 and herpetic lesions13,14 have also been reported. However, there is still no evidence that these lesions are caused directly by the virus.1
Our objective was to characterize oral lesions and associated clinical findings in COVID-19 patients.
MethodsThe study population consisted of hospitalized patients (n = 55) with COVID-19 confirmed by polymerase chain reaction (PCR) and a rapid antigen fluorescent immunoassay (FIA) diagnostic test. All patients had moderate or severe disease.
After obtaining informed consent, the medical history of each patient was reviewed and an examination of the oral cavity was performed. Each patient was questioned to evaluate taste disturbances and xerostomia. The clinical findings of the oral examination were recorded in a database designed specifically for this purpose. In cases in which oral lesions required medical treatment, this was recorded.
Data were analyzed using descriptive statistics. The variable “age” was compared using the Student’s t-test and P-values <0.05 were considered statistically significant.
ResultsThe study population consisted of 30 men (54.5%) and 25 women (45.5%), ranging in age from 1 to 89 years (mean ± standard deviation, 51 ± 23.24 y) All patients were hospitalized and 19 (34.5%) were admitted to the intensive care unit (ICU). All patients in the ICU were treated with dexamethasone and remdesivir. Most of the patients hospitalized in the ward received antiviral therapy consisting of a combination of lopinavir and ritonavir.
Patients with no underlying disease accounted for 45.5% of the study population. In those with underlying disease, hypertension was the most common disease (18.2%), and 10.9% had hypertension with concomitant diabetes. Asthma was another frequently recorded disease (16.4%). Recorded past history included hepatitis and oncological processes.
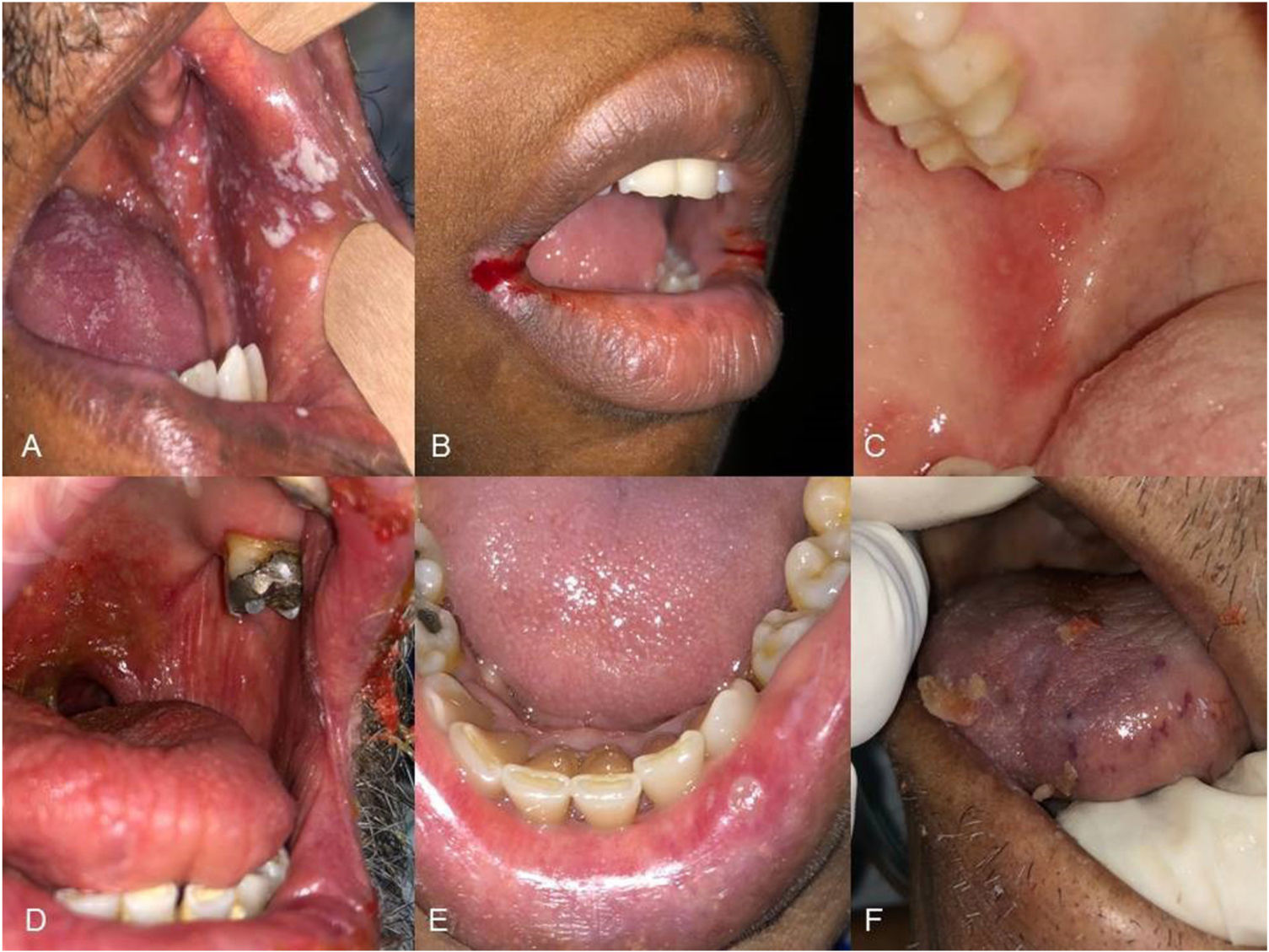
In 22 patients (40%) at least one alteration or lesion was observed in the oral mucosa (Figs. 1 and 2). Erythematous and pseudomembranous forms of candidiasis were diagnosed in 7 patients (12.7%), and severe angular cheilitis in 1 patient (Fig. 1B). All were treated with topical and systemic antifungals. The patient with angular cheilitis was treated with a topical mixture consisting of an antibiotic and an antifungal.
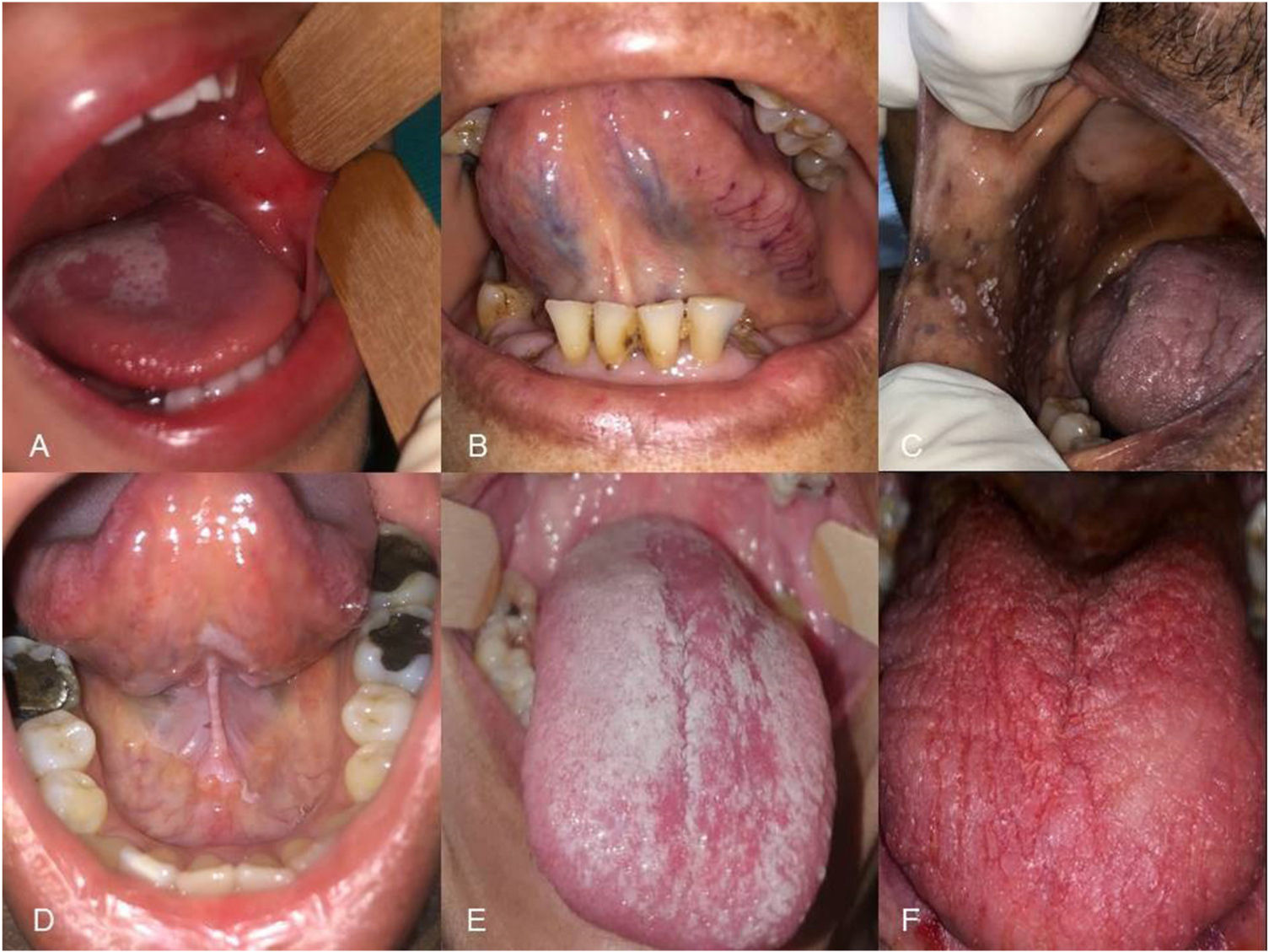
Oral lesions in COVID-19 patients. A, Migratory glossitis and petechiae on the cheek. B, Unilateral caviar tongue. C, Pseudomembranous candidiasis. D, Leukoplakia on the floor of the mouth and the ventral aspect of the tongue (non-smoker). E, Pseudomembranous candidiasis. F, Erythematous candidiasis.
Hemorrhagic ulcerative lesions were observed in 4 patients (7.3%) and multiple ulcerations resembling canker sores in 3 patients (5.5%). Two patients presented enanthems in the labial or cheek mucosa (Figs. 1C and 2A).
Other observed lesions included white plaques (1 patient) and lichenoid lesions (1 patient). In these cases a biopsy was indicated after recovery from the viral infection.
Finally, 1 patient developed a recurrent cold sore, 3 had lingual varicose veins, and 3 were diagnosed with migratory glossitis, onset of which may or may not have occurred before COVID-19.
Oral lesions were more common in men than in women (13 and 9 cases, respectively), although there was no significant difference between the 2 groups (P = 0.58, Pearson’s χ2 test). There was no significant difference in mean age between the patients with lesions and those without (53.45 ± 22.51 and 49.36 ± 23.92 y, respectively; P = 0.52). Only 6 (27.3%) of the 22 patients with oral manifestations were admitted to the ICU.
Alteration or a total loss of taste was recorded in 33 patients (60%), pain or burning in the mouth in 20 patients (36.4%), and xerostomia in 15 patients (27.3%). Both dysgeusia and oral pain or burning were common in patients with mucosal lesions (68.2% and 77.3%, respectively).
DiscussionEmerging evidence has sparked much debate regarding the true relationship between oral manifestations in COVID-19 patients and the viral infection itself. The first descriptions of the oral mucosa in COVID-19 patients, recorded in Spain, primarily described ulcerative lesions, similar to those associated with herpetic infections.13
It has been suggested that oral ulcers may be an initial sign of viral infection.15,16 In our study, ulcers were the most commonly observed lesions and included both hemorrhagic and aphthous-like lesions. None of our patients underwent biopsies to detect viral proteins in the affected tissue, although the presence of viral spike protein in the oral cavity has been reported,4 suggesting that these ulcers may be due to tissue damage caused directly by the virus. Vascular damage revealed in histological studies of oral cavity lesions suggests that oral lesions may be a consequence of thrombotic vascular damage in the mucosa and subsequent vasculitis.10,17
Enanthem-type lesions have also been described in COVID-19 patients.6,18,19 These include petechiae, erythematous macules, and erythematous–vesicular patterns in the oral mucosa, often associated with secondary viral clinical signs.6 In our study, enanthem-type lesions were only observed in 1 child and 1 adult, and were accompanied by intense pain, which may be associated with the tissue damage caused by the virus.
Manifestations secondary to viral infection were frequently observed in the buccal mucosa of our patients. Candidiasis and recurrent herpetic infection are common lesions in COVID-19 patients.20 A causal relationship between viral infection and these lesions cannot be established: their appearance seems to constitute a secondary response to drug treatment, immune system alterations, and high levels of stress caused by viral infection.11
Caviar tongue and geographic tongue were also recorded in our COVID-19 patients, although these entities are quite common in the general population. A limitation of the present study is that it was impossible to accurately determine the moment of onset of these alterations and therefore to directly relate these changes to COVID-19.
Finally, changes in taste perception and oral burning or pain were very frequent, and were also associated with the appearance of oral lesions. Taste disorders can be a significant and specific clinical sign of COVID-19, and may even constitute an early marker of viral infection.1
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Villarroel-Dorrego M, Chacón L, Rosas R, Barrios V, Pernía Y, Vélez H. Hallazgos bucales en pacientes COVID-19. Actas Dermosifiliogr. 2022;113:183–186.