Laser and light-based therapies play a significant role in the management of erythematotelangiectatic rosacea (ETR), which frequently exhibits minimal response to medical therapies.1 Furthermore, research into treatment of rosacea vascular manifestations have often shown an improvement of the papulopustular component too, probably due to the immunomodulatory effects of light therapies.2 This study aims to evaluate the safety and efficacy profile of a novel device that incorporates variable-sequenced, long-pulsed, 532-nm potassium titanyl phosphate (KTP) and 1064-nm neodymium:yttrium–aluminum–garnet (Nd:YAG) lasers with cryogen spray cooling (DermaV, Lutronic®) in patients with ETR.
We conducted a retrospective observational cohort study at the Department of Dermatology of Hospital Ramon y Cajal (Madrid, Spain). Our study included a total of 25 patients with ETR with or without papulopustules were treated with the above-mentioned device from December 2022 to September 2023. The mean age was 51.7±14.9 years, 72% were women with Fitzpatrick skin type II (72%) or III (28%) (Supplemental Table 1). The median number of sessions was 2 (range 1–5), with a median passes per session of 2 (range 1–6) and a median inter-session interval of 3.7 weeks (IQR, 3–5). Treatment parameters were left at physician's discretion based on previous experience and clinical endpoints during treatment. Table 1 illustrates laser parameters and Supplemental Fig. 1 depicts pulse modes. Three independent dermatologists evaluated pre- and post-treatment patient photographs and assessed the Investigator's global assessment (IGA) at baseline and 8–12 weeks after treatment, as well as an adapted IGA evaluating erythema, telangiectasias and papulopustules separately. Observers also rated the baseline improvement after treatment on a 5-point ordinal scale: none/worsening (0%); poor (1–25%); mild (25–50%); good (50–75%) and excellent (>75%). Patients reported their degree of satisfaction as very satisfied, satisfied, or dissatisfied, and procedural pain using a visual analog scale from 0 (no pain) up to 10 (extremely painful). Finally, safety and adverse events were collected.
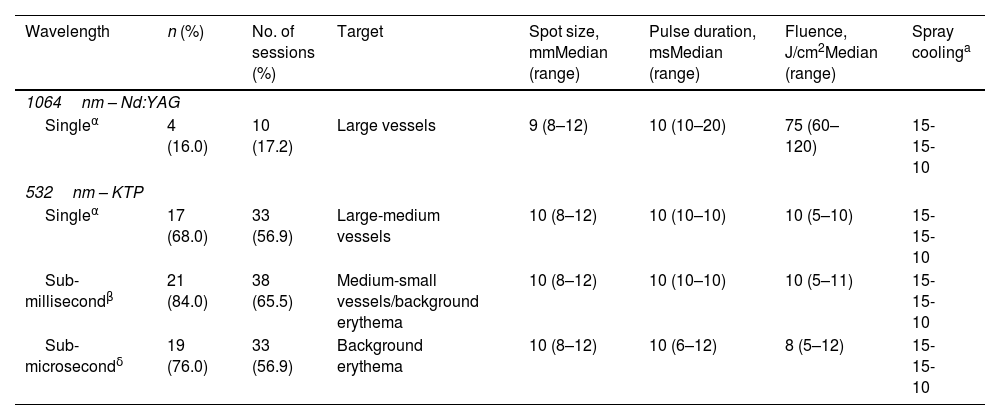
Laser parameters used.
| Wavelength | n (%) | No. of sessions (%) | Target | Spot size, mmMedian (range) | Pulse duration, msMedian (range) | Fluence, J/cm2Median (range) | Spray coolinga |
|---|---|---|---|---|---|---|---|
| 1064nm – Nd:YAG | |||||||
| Singleα | 4 (16.0) | 10 (17.2) | Large vessels | 9 (8–12) | 10 (10–20) | 75 (60–120) | 15-15-10 |
| 532nm – KTP | |||||||
| Singleα | 17 (68.0) | 33 (56.9) | Large-medium vessels | 10 (8–12) | 10 (10–10) | 10 (5–10) | 15-15-10 |
| Sub-millisecondβ | 21 (84.0) | 38 (65.5) | Medium-small vessels/background erythema | 10 (8–12) | 10 (10–10) | 10 (5–11) | 15-15-10 |
| Sub-microsecondδ | 19 (76.0) | 33 (56.9) | Background erythema | 10 (8–12) | 10 (6–12) | 8 (5–12) | 15-15-10 |
KTP: potassium titanyl phosphate; Nd:YAG: neodymium:yttrium–aluminum–garnet; α: continuous pulse; β: pulse duration is subdivided into 1.5ms sub-pulses in succession; δ: pulse duration is subdivided into 0.3ms sub-pulses in succession.
The device allows cooling delivery before and after laser pulse. First value depicts duration of cooling delivery in ms, second value the time prior to pulse delivery, and the third value time of post-cooling in ms (e.g., 15-15-10: 15ms of cryogen spray, delivered 15ms prior to laser pulse, with 10ms post-cooling spray).
IGA reduced significantly after treatment (Table 2), being global IGA improvement significantly associated with the number of sessions (β=0.59; p=0.003). There was subjective clinical improvement>50% in 73.3% of cases. Notably, high inter-observe agreement was reported, with weighted kappa coefficients from 0.56 up to 0.74 (p<0.05) (Supplemental Table 2). The median intraoperative pain score was 6 (IQR, 4–7). The most commonly reported adverse event was edema (76% of patients), with a median duration of 3 days (range, 1–10). No purpura was observed. One patient exhibited transient post-inflammatory hyperpigmentation (Fig. 1C). All patients reported that temporary discomfort was tolerable. Finally, 32% of patients reported being very satisfied, 56% being satisfied and 12% being dissatisfied.
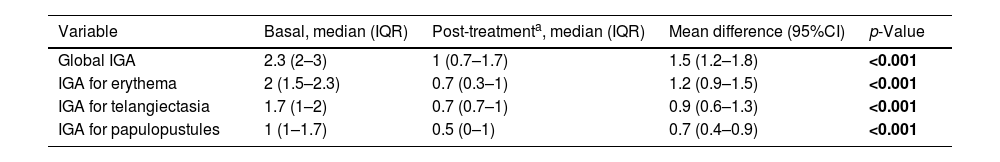
Investigator Global Assessment change after treatment.
| Variable | Basal, median (IQR) | Post-treatmenta, median (IQR) | Mean difference (95%CI) | p-Value |
|---|---|---|---|---|
| Global IGA | 2.3 (2–3) | 1 (0.7–1.7) | 1.5 (1.2–1.8) | <0.001 |
| IGA for erythema | 2 (1.5–2.3) | 0.7 (0.3–1) | 1.2 (0.9–1.5) | <0.001 |
| IGA for telangiectasia | 1.7 (1–2) | 0.7 (0.7–1) | 0.9 (0.6–1.3) | <0.001 |
| IGA for papulopustules | 1 (1–1.7) | 0.5 (0–1) | 0.7 (0.4–0.9) | <0.001 |
The final IGA for each patient was the mean of the IGA provided by each of the independent evaluators. With these final IGAs, the baseline and post-treatment IGA of the sample are calculated.
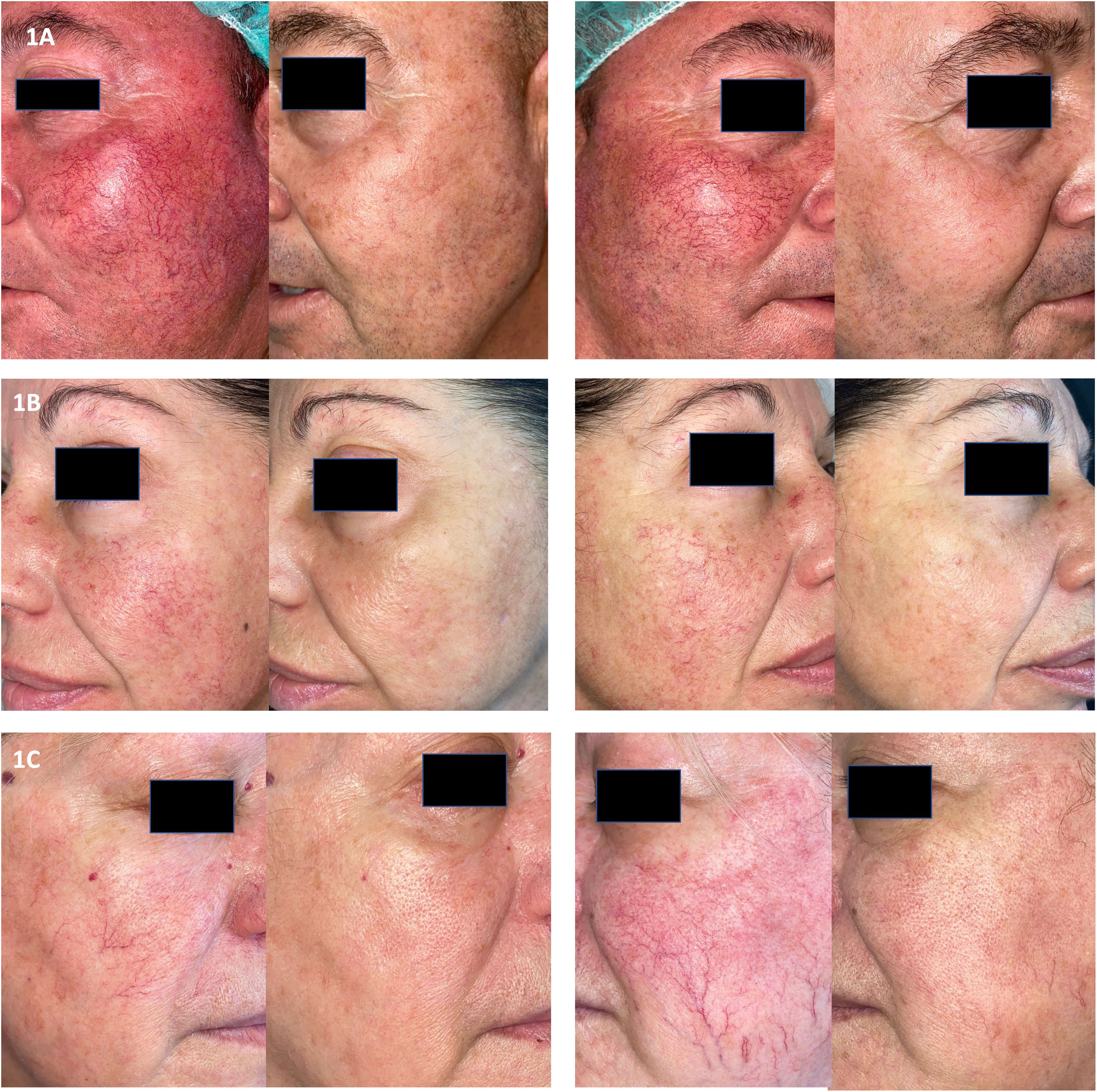
Examples of pre- and post-treatment photographs of patients. (A) The patient received 4 sessions. The first one with Nd:YAG for tracing larger telangiectasias (8mm spot, pulse duration 20ms with single mode, fluence 60J/cm2), followed by KTP 10mm, 10ms on single mode and 10J/cm2. A second session with similar parameters was conducted, followed by 2 sessions of 2 passes of KTP laser in a single sub-millisecond mode; (B) Patient received 5 sessions of KTP laser in a single pulse mode (10ms) for medium telangiectasia, with a spot of 12mm and a fluence ranging 7–8J/cm2, followed by KTP on sub-microsecond pulse mode (10ms) with a 10mm spot size and a fluence of 8J/cm2 for background erythema; (C) Results after 5 sessions. Nd:YAG was used for tracing larger telangiectasias (spot 8mm, pulse duration 10ms with single mode, fluence ranging 70–120J/cm2) followed by KTP single mode (10ms, spot 10–12mm and fluence of 10J/cm2) for medium vessels and sub-millisecond and submicrosecond modes (spot size 10–12mm, fluence 8–10J/cm2 and pulse duration 10ms) for small vessels and diffuse erythema. A slight hyperpigmentation was observed after session 5 that resolved within the next few weeks.
The novel, variable-sequenced, laser device used in the current study showed an adequate safety and effective profile in treating the telangiectasias, redness and papulopustules that characterize rosacea. These results were consistent with those reported by Bernstein in a recently published work that included 19 patients with ETR treated with the same device.3 A mean improvement of 39% was observed, being edema the most frequently reported adverse effect. In a study including 23 patients with pigmented and vascular lesions—diagnosis not provided—86.4% were considered responders.4 Compared to previous KTP laser devices, the combination of 2 wavelengths and specially the different pulse structures available provides a greater capacity to adapt to the thermal relaxation times of the different vascular structures typical of rosacea, increasing its versatility. Additionally, by increasing the number of pulses delivered, sub-millisecond and sub-microsecond pulse modes increase peak power while maintaining fluence, pulse duration and spot size. This may be particularly important on subsequent treatments, when chromophore decrease forces to increase fluence and, frequently, to reduce the spot size. Maintaining beam diameter ensures an adequate depth of laser penetration and enables faster treatments. Finally, compared to contact cooling, cryogen spray cooling avoids the risk of compressing blood vessels, thus reducing the chromophore and enables a more comfortable treatment of the nasal ala. Further research is needed to firmly establish the optimal laser parameters based on the vessel morphology, and compare this device with pulsed-dye laser, which is considered the treatment of choice for vascular lesions of rosacea.5 Limitations of the study include its small sample size and retrospective nature.
Conflict of interestThe authors declare that they have no conflict of interest.