Trigeminal trophic syndrome (TTS), also known as trigeminal neurotrophic ulceration, is a rare condition that occurs when the trigeminal nerve is damaged. It presents with anesthesia or unilateral dysesthesia that typically affects the ala nasi, and with ulcerations that are self-inflicted, usually unconsciously, by the patient.1
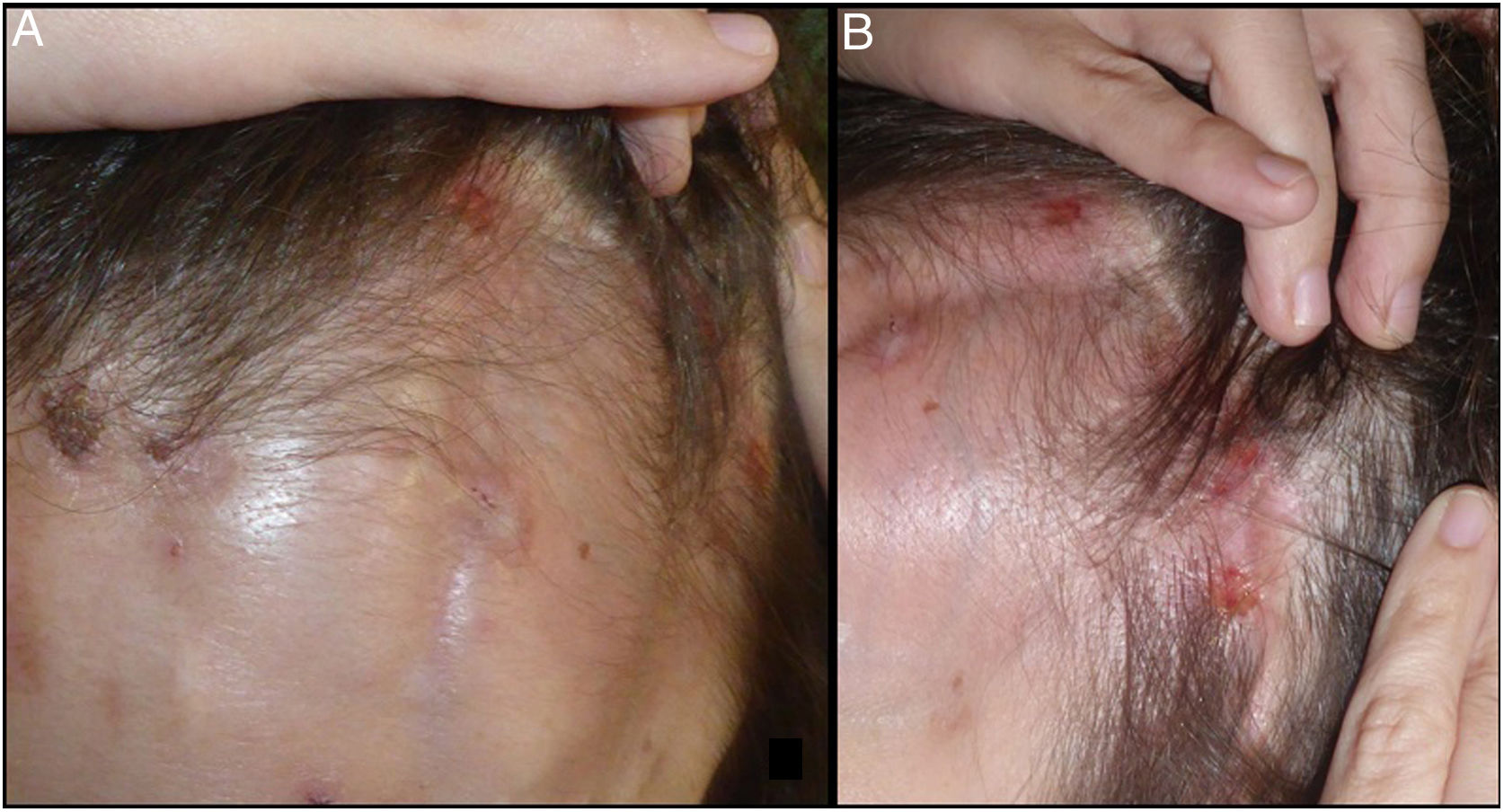
A 38-year-old woman was examined for pruriginous erosive and mildly painful lesions that had appeared 2 months earlier in the left frontoparietal region. The patient had undergone surgery for a meningioma measuring 46 × 40 × 38 mm in the left cavernous sinus a year and a half earlier by means of frontotemporal cutaneous incision and left pterional craniotomy. Since the surgery, the patient had presented sequelae including paresis of cranial nerves III and IV in the left eye, neurotrophic keratitis in the left eye, and panhypopituitarism with secondary hypogonadism and hypothyroidism. The last follow-up imaging study performed a month before visiting our department and approximately a month after onset of the skin condition, showed a recurrence of the meningioma in the left cavernous sinus. The patient had been examined a month earlier at the ophthalmology department for an episode of herpes zoster that involved the V1 branch of the trigeminal nerve, with no ophthalmologic involvement. Without microbiologic confirmation, she received treatment with valaciclovir and was sent to our department due to the persistence of the lesions when the treatment had been completed. When she visited our department, she presented several crusted erosive lesions of varying morphology on a background of hypersensitive atrophic skin compared to the contralateral region (Fig. 1). We reached a diagnosis of TTS, with ulcers secondary to dysesthesia and anesthesia in the left V1 region, probably linked to the recurrence of meningioma. Treatment was instated at that time with tacrolimus cream, 0.01% and covered with a hydrocolloid dressing. The patient was also offered the option of starting treatment with oral gabapentin, which se rejected. After 2 months of treatment, the lesions improved considerably.
TTS is characterized by the presence of unilateral facial ulcers caused by persistent scratching as a result of the dysesthesia (described as itching, or a burning or tingling sensation) and anesthesia in the sites innervated by the previously damaged trigeminal nerve or one of its branches. Patients often scratch to alleviate the feeling of discomfort and, due to the anesthesia, cause persistent ulceration. A systematic review of the literature in by Sawada et al. in 2014,2 which included 61 cases of TTS published to that date, describes the principal etiologies of this syndrome. The most commonly reported causes are ablation of the trigeminal nerve (30%), cerebrovascular accident (30%), and surgical complications, including a history of craniotomy (21%). Another, less frequently reported cause is herpes zoster, which is also mentioned by other authors, such as Dolohanty et al.,3 who describe development of TTS in the V1 region 2 months after an episode of herpes zoster in the same dermatome, which was treated with valaciclovir. In our case, we believe that the initial clinical presentation, diagnosed as herpes zoster, was probably the onset of TTS.
Furthermore, damage to the trigeminal nerve may occur in up to 11% of patients who undergo surgery for meningioma.4 The first case of TTS associated with meningioma was described in 1982.5 Three further publications link TTS and meningioma surgery, although in one of them, the TTS appeared after surgery for a recurrence of the meningioma 9 years after the primary tumor.6 Thus, although our patient potentially presents 3 of the etiologic factors most frequently associated with development of TTS (meningioma, craniotomy and a doubtful episode of herpes zoster), we believe that the sequence of appearance of the symptoms and the coincidence with the recurrence of the meningioma make the meningioma the most probable cause.
In terms of treatment of TTS, improvement of cutaneous symptoms has been reported with tacrolimus cream, 0.01%, gabapentin, and hydrocolloid dressing.7 Improvement of the lesions has also been observed after use of high doses of carbamazepine (200 mg/3 times daily).8 Other drugs, such as amitriptyline, pregabalin, and alprazolam have been used with little or no clinical benefit.
Conflicts of interestThe authors declare that they have no conflicts of interest.
Please cite this article as: Fernández-Bernáldez A, et al. Síndrome trófico trigeminal secundario a recidiva de meningioma. Actas Dermosifiliogr. 2020;111:171–173.